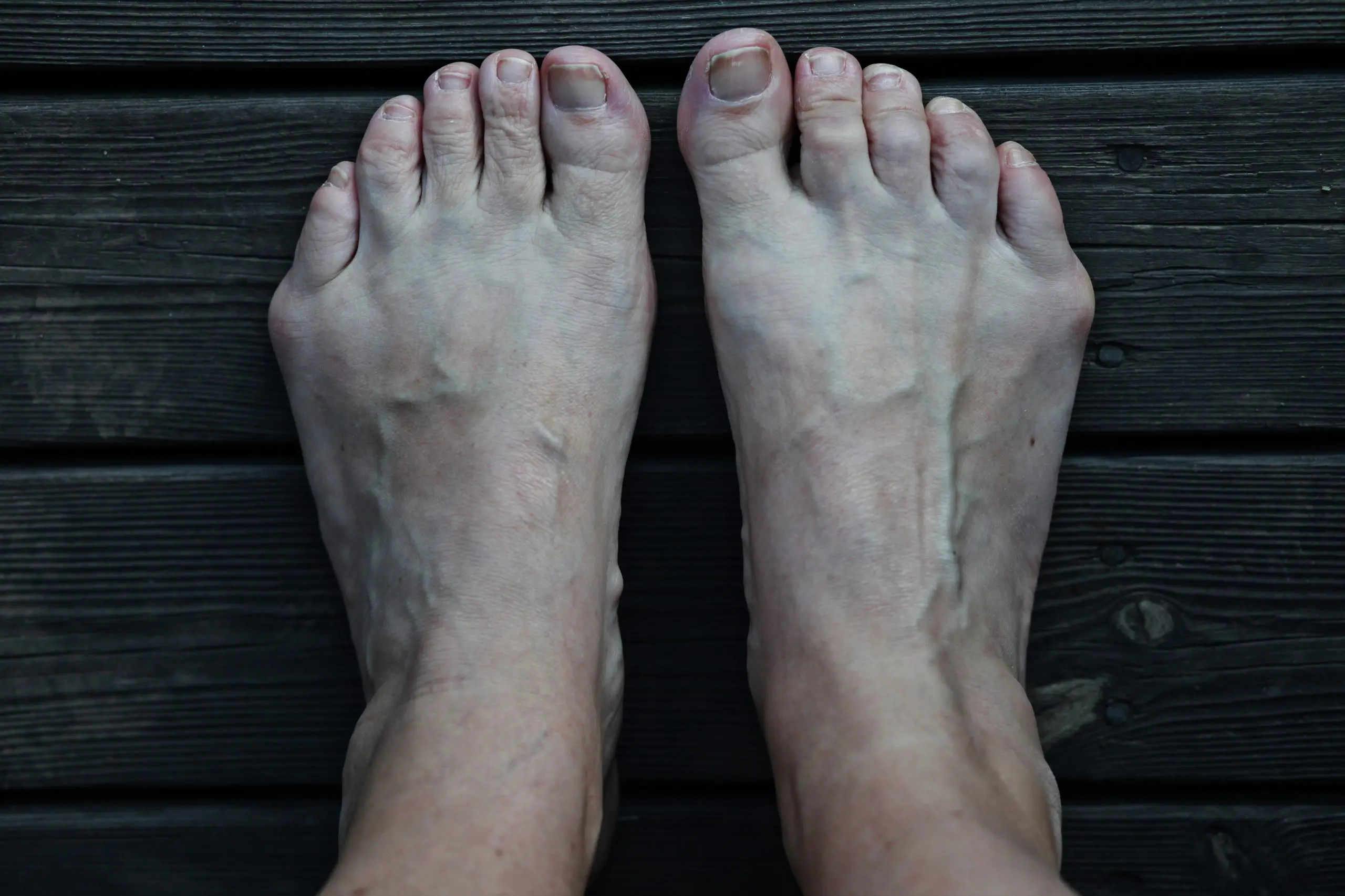
The bunionette, also known as quintus varus or tailor’s bunion, is a toe deformity caused by a deformation of the 5th metatarsal bone.
Mirroring the bunion of the foot (hallux valgus), the bunionette causes a deviation of the last toe that makes it difficult to put on the shoe.
This foot condition, if not treated properly, can cause extreme discomfort and consequences, which can be life-threatening in some cases.
It’s important to understand the conditions surrounding a quintus varus in order to see a podiatrist as soon as possible.
You can find the symptoms, causes, and remedies for a bunionette here.
Symptoms and complications
Even though the bunionette is easy to identify from other toe abnormalities like hallux valgus or hammertoes, knowing how to recognize it is vital for preventing further complications.
This type of metatarsalgia provides esthetic discomfort as well as a variety of symptoms, including:
- Noticeable pain in the joint of the little toe;
- Difficulty getting dressed comfortably;
- Thickening of the skin in the affected area;
- Outward deviation of the base of the affected toe;
- Redness and swelling;
- Considerable stiffness in the toe;
- Accumulation of corns or calluses at the base of the toe.
The bunion will most certainly worsen if it is not treated effectively.
The resulting complications can be quite inconvenient, and even serious:
- Chronic pain;
- Acute inflammatory bursitis;
- An enlargement of the bony deviation, to the point of retraction of the toe;
- The appearance of a wound;
- Osteoarthritis;
- Inflammation of the phalanx bone (osteitis);
- A dislocation of the joint.
Obviously, if the foot is treated as soon as the initial symptoms arise, the odds of severe consequences happening are slim.
An infected wound, on the other hand, might be extremely harmful for someone who already has a condition, like diabetic foot.
Causes and aggravating factors
The bunionette occurs due to complementary bony abnormalities.
In the first, the metatarsal bends outward and forms a prominence. In the second, the last phalanx of the little toe curves inward and approaches the adjacent toes.
A number of reasons can be attributed for these joint deformities:
- A flat foot or a cavus foot;
- A foot malformation that is present from birth;
- An inflammatory disease such as rheumatoid arthritis;
- Aftereffects of a stroke on the nervous system;
- A foot trauma caused by a shock or one that has not been properly treated;
- Wearing shoes that aren’t right for your feet and don’t leave enough room for your toes;
- Frequent wearing of high heels;
- Playing a sport that increases the stress on the little toe, such as skiing or ballet.
Bunionette prevention
The bunion, as we’ve seen, must be addressed medically as soon as possible.
However, there are a few preventative steps that can assist to mitigate the effects:
- Maintain a healthy body mass index (BMI).
- Reduce the amount of time you spend wearing high heels.
- Purchase shoes with broad ends that do not squeeze your toes.
- Avoid walking barefoot or wearing sandals or moccasins, which are overly flexible.
- Wear prefabricated orthopedic insoles or a protective device placed near the joint.
If this initial treatment isn’t enough to keep the bunionette at bay, consult a podiatrist for a diagnosis and treatment.
Medical treatments
Treatment for bunionette should largely focus on treating the mechanical imbalance that causes the deformity.
However, before recommending a solution, the podiatrist will do a series of tests to determine the source of the problem.
These tests can include:
- Biomechanical examination of the foot;
- Postural assessment of the foot;
- Visual auscultation of the foot;
- Digital radiography;
- Ultrasound of the foot.
The podiatrist designs a treatment strategy to lessen the consequences of quintus varus once the diagnosis and etiology have been determined.
The following methods are commonly used to treat the bunionette:
- An orthosis for the toe (orthoplasty);
- Custom-made foot orthoses;
- Orthopedic shoes;
- Prescription of anti-inflammatory medications;
- If the joint is affected, cortisone injection;
- Manual foot therapy;
- Foot care, which includes soaking, softening, moisturizing the feet, and removing partridge eyes (advanced form of corns on the foot).
If the bunionette persists, more invasive procedures to control its progression may be recommended.
We then consider foot surgery:
- Metatarsal osteotomy, which involves cutting the bone that is causing the protruding deformity;
- Percutaneous surgery, which is much less invasive and requires only small incisions in the foot.
Typically, the podiatrist will do all in their ability to avoid surgery, which requires a long-term remission.
PiedReseau – Learn more
Do you want to learn more about the bunionette? We have a lot of information on toe abnormalities on our site!
On the other hand, while the PiedReseau website contains useful information, nothing matches a face-to-face consultation with a podiatrist.
Take care of your feet, they’re precious!
A bunionette is a foot malformation in the fifth toe (little toe). This bony protrusion is frequently uncomfortable and inflammatory.
A bunionette of the foot can be produced by a flat or cavus foot, a congenital foot deformity, or by wearing improperly fitting shoes. The usage of high heels on a regular basis might also be a contributing factor.
Quintus varus comes in two varieties. The first occurs when the little toe is situated higher than the fourth toe. The second condition occurs when the little toe is beneath the fourth toe.
Quintus varus (bunionette) is the little toe’s malformation. The big toe’s malformation is called the hallux valgus. Hammer toe is a curvature of the toe that is frequently in the shape of an inverted “V” and generally affects the second, third, and fourth toes of the foot.
Bunionette can cause persistent discomfort and irritation if left untreated. The bony distortion can sometimes become so severe that the toe retracts or the joint dislocates. Furthermore, if you have diabetes, the effects of a bunionette might be quite troublesome. If an infected lesion develops, the bunionette may need foot amputation. As a result, it is best to take care of it as quickly as possible!
Depending on the situation, the recovery period following surgical treatment for quintus varus is around 2 months.