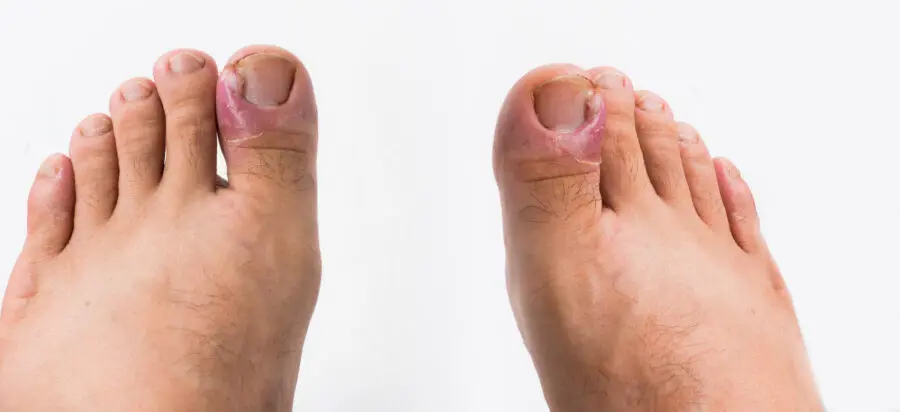
Much like the ingrown nail, paronychia involves inflammation or infection of the cuticle of a toenail.
The inflammation of the skin around the affected nail is often caused by the bacterium Candida albicans (candidiasis thrush).
This results in a throbbing pain, redness and swelling of the affected toe.
If left untreated, this condition can eventually lead to pus accumulation and infection that spreads further to the toe or even the foot.
Learn more about the medical treatments for paronychia available at podiatry clinics.
Drainage
As mentioned earlier, when the foot contacts a candidiasis-like bacteria, it can develop an infection of the cuticle.
As a result, this infection can lead to the accumulation of pus under the top layer of skin.
In this case, the podiatrist may suggest treating the purulent area with drainage.
Usually drainage of the subungual abscess happens as follows:
- The podiatrist asks the affected patient to lie down
- The painful area is anesthetized
- The podiatrist carefully separates the infected skin from the nail using a sterile tool
- The podiatrist punctures the abscess with a sterilized needle to allow the pus to drain out
Although it may be tempting to perform this procedure yourself, you are strongly discouraged from doing so.
This could expose other areas of the foot to infection.
Take foot baths
Soaking the feet temporarily softens the skin and cuticles.
It is used to facilitate the natural continuation of drainage after the operation at the clinic.
Typically, you should soak the foot for the treatment of paronychia like this:
- The water is hot enough to increase blood circulation but cold enough not to burn the skin
- One soaking session lasts 15 minutes
- The frequency of soaking the toe is 3 to 4 times per day
- It is recommended to wear a protective bandage between soaking sessions
If the normal healing process does not begin after a few days or the pus continues to flow, we advise you to visit the podiatrist again.
Prescription antifungals
Although the occurrence of paronychia is more often attributed to the bacterium Candida albicans, it can also be caused by a fungus.
Therefore, in both acute and chronic paronychia, it is occasionally necessary to supplement treatment with a prescription of antifungal agents.
The prescription of antibiotics
Usually, you can get an over-the-counter antibacterial cream to treat paronychia in the early stages.
If the patient chooses this type of ointment, they should apply the cream topically after soaking the feet, twice a day.
However, if the paronychia is discovered later, there may be need for antibiotic treatment.
Foot care
Clinical foot care both relieves the discomfort of paronychia and reduces the likelihood that it will recur.
Some of the foot treatments available at the clinic include:
- Topical application of special creams
- Medical trimming and sizing of toenails
- Therapeutic and antiseptic foot baths
Complete or partial removal of the nail
Poor care and deformation of toenails play a major role in the development of paronychia.
These not only favor its occurrence, but can also facilitate its return.
This more invasive procedure involves removing the problematic portion of the nail and then chemically burning the root to provide permanent protection.
However, complete or partial removal of the toenail is still a last resort treatment.
Orthopedic shoes
Wearing shoes that do not fit the shape of the foot is one of the main causes of recurrent paronychia.
For instance, if a shoe is too tight or does not properly support the foot, it exposes the toes and nails to more pressure points.
Improper shoes subject your toes to repetitive stress and thus increase the likelihood that the nails will deform or flake.
Therefore, in order to protect the foot, the podiatrist may suggest prescribing orthopedic shoes that are appropriate for the particular plantar characteristics of his patient.
The foot pathologies that may cause the podiatrist to suggest this orthopedic device are:
- The flat or cavus foot
- Bunion (hallux valgus)
- Hammertoes
- Clubfoot
PiedReseau – Learn more
Want to learn more about bacterial and fungal infections of the foot like paronychia? Our site has an abundance of information on this subject!
But even though the PiedReseau website offers valuable insight, nothing is better than a real consultation with your podiatrist.
Take care of your feet, they are precious!